It’s a common assumption, one often repeated with a knowing nod: stained teeth are a sure sign that someone’s slacking on their brushing and flossing. While it’s undeniably true that neglecting oral hygiene can lead to a buildup of plaque and tartar which can discolor teeth, the narrative that all tooth stains stem from poor hygiene is a pervasive myth. The reality is far more nuanced, with a surprising array of factors contributing to the shade of our smiles, many of which have absolutely nothing to do with how diligently we wield our toothbrushes.
Let’s first acknowledge where hygiene plays its part. When we don’t brush and floss effectively, a sticky film of bacteria called plaque forms on our teeth. If left undisturbed, plaque hardens into tartar (or calculus), which is often yellow or brown. Furthermore, plaque can readily absorb pigments from foods and drinks, leading to surface stains. So yes, consistent, thorough oral hygiene is a cornerstone of maintaining not only healthy teeth and gums but also a brighter appearance by keeping these superficial culprits at bay. However, to stop the investigation there would be to ignore a host of other influential elements.
The Wider World of Tooth Discoloration: Extrinsic Culprits
Beyond basic plaque accumulation, many external factors, known as extrinsic stainers, can alter the color of our tooth enamel. These are substances that come into contact with the tooth surface.
Your Daily Plate and Cup
Think about your daily diet. That morning cup of coffee or tea, the glass of red wine with dinner, or even certain deeply colored fruits and vegetables can leave their mark. These items often contain potent color molecules called chromogens that have a knack for sticking to tooth enamel. Tea and red wine are also rich in tannins, compounds that can make teeth more susceptible to staining by helping chromogens adhere. Even seemingly healthy foods like berries (blueberries, blackberries, pomegranates), vibrant sauces (soy sauce, tomato-based sauces, curry), and some candies or sports drinks can contribute to a less-than-pearly white smile over time. The acidity of some foods and drinks can also erode enamel, making the surface rougher and more prone to picking up stains.
The Impact of Tobacco
It’s no secret that tobacco use is detrimental to overall health, and dental aesthetics are no exception. Both smoking and chewing tobacco introduce tar and nicotine into the mouth. While nicotine is colorless on its own, it turns yellow when it reacts with oxygen. Tar, by its very nature, is dark. These substances seep into the microscopic pores of the enamel, causing stubborn yellow or brownish discoloration that can be very difficult to remove with brushing alone.
Delving Deeper: Intrinsic Stains from Within
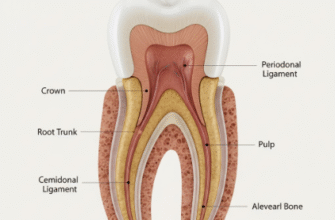
Perhaps more surprising are intrinsic stains. These occur from within the tooth structure itself, affecting the dentin (the layer beneath the enamel) or the enamel as it develops. Because these stains are internal, they are generally more resistant to regular brushing and over-the-counter whitening products.
When Medicine Leaves Its Mark
Certain medications are known culprits for intrinsic staining. The antibiotic tetracycline and its derivatives (like doxycycline and minocycline) are notorious for this. If taken by pregnant women during the second half of pregnancy, or by children whose teeth are still developing (typically up to the age of 8), these antibiotics can bind to the calcium forming the teeth, resulting in permanent greyish-brown or yellowish banding. Even some antihistamines (like Benadryl), antipsychotic drugs, and medications for high blood pressure can occasionally contribute to tooth discoloration in adults, though typically to a lesser extent.
The Unseen Effects of Medical Interventions
Certain medical treatments can also impact tooth color. Chemotherapy and radiation therapy, particularly when directed at the head and neck, can sometimes cause discoloration. These treatments can affect the cells responsible for tooth formation if teeth are still developing, or they can alter the existing tooth structure or saliva flow in ways that predispose teeth to staining.
Too Much of a Good Thing? Fluoride’s Role
Fluoride is a champion in preventing tooth decay, but excessive exposure to it during the years of tooth formation (again, primarily in childhood) can lead to a condition called dental fluorosis. This condition can manifest as faint white lines or flecks on the enamel in its mildest forms. In more severe cases, which are rarer, fluorosis can cause more noticeable opaque white patches, or even brown, pitted, and mottled enamel. The critical period for fluorosis development is generally before the age of 8, when permanent teeth are forming under the gums.
The Aftermath of Injury
Trauma to a tooth, such as from a fall or a sports injury, can cause it to change color. If the nerve and blood supply to the tooth are damaged, the tooth might die. As the internal tissues break down, pigments can be released that permeate the dentin, often leading to a grayish, pinkish, dark yellow, or even black appearance. This discoloration can happen weeks, months, or even years after the initial injury.
The Natural March of Time: Aging
As we age, our teeth naturally tend to appear more yellow. This is due to two primary factors. First, the outer layer of enamel gradually wears down over decades of chewing, grinding, and exposure to acidic foods. This thinning enamel allows more of the underlying dentin to show through. Dentin is naturally yellower and less translucent than enamel. Second, dentin itself can also change and darken over time through a process called secondary dentin formation.
The Genetic Lottery
Sometimes, the baseline color of your teeth is simply down to genetics. Just as genes determine our hair and eye color, they also play a role in the natural thickness and translucency of our enamel, as well as the inherent shade of our dentin. Some people are born with brighter or thicker enamel than others, making their teeth appear naturally whiter. Conversely, some may have thinner enamel or a more yellowish hue to their dentin from the get-go, irrespective of their hygiene habits or diet.
Understanding the Stain Spectrum
Recognizing the difference between extrinsic and intrinsic stains is key. Extrinsic stains, being on the surface, are often manageable with diligent home care, professional cleanings, and sometimes over-the-counter whitening products. Intrinsic stains, originating from within the tooth, are generally more challenging and may require more advanced cosmetic dental procedures like professional-strength bleaching, bonding, or veneers if a color change is desired.
Verified Information: Tooth discoloration is a complex issue with a multitude of causes. While poor oral hygiene can contribute to surface stains, factors like diet, medications, aging, trauma, and even genetics play significant roles. Identifying the specific cause of tooth staining is crucial for determining the most effective approach to manage or improve it.
Navigating Towards a Brighter Smile
So, if your teeth aren’t as white as you’d like, don’t automatically assume it’s a failing on your part regarding brushing and flossing. While maintaining excellent oral hygiene is paramount for overall dental health and preventing some types of surface stains, it’s not a universal antidote to all discoloration.
Preventative Measures and Professional Help
For extrinsic stains, certain lifestyle adjustments can help. Moderating intake of staining foods and drinks, rinsing your mouth with water after consuming them, and, of course, avoiding tobacco are good preventative steps. Regular dental check-ups and professional cleanings are also vital. A dental hygienist can remove plaque, tartar, and many superficial stains that home care might miss, significantly brightening your smile.
Addressing Existing Discoloration
If stains persist, various options exist. For many extrinsic and some milder intrinsic stains, professional teeth whitening (either in-office or custom take-home trays from your dentist) can be effective. Over-the-counter whitening products like strips or toothpastes may offer some improvement for very light surface stains, but their efficacy is generally limited compared to professional treatments. For deeper, more resistant intrinsic stains, cosmetic procedures such as dental bonding (applying a tooth-colored resin to the tooth surface) or porcelain veneers (thin shells custom-made to cover the front surface of teeth) might be considered.
The Importance of a Dental Consultation
The most important step if you’re concerned about tooth discoloration is to consult with your dentist. They can perform a thorough examination to help determine the underlying cause of the staining – whether it’s extrinsic, intrinsic, or a combination. Once a cause is identified, your dentist can discuss the most appropriate and effective treatment options tailored to your specific situation, needs, and budget. They can also advise on whether a particular type of stain is likely to respond to whitening or if other cosmetic solutions would be more suitable.
Concluding Thoughts: Beyond the Brush
The color of our teeth is influenced by a rich tapestry of factors, extending far beyond the reach of our toothbrush bristles alone. While stellar oral hygiene is a non-negotiable foundation for a healthy mouth and can help ward off some common surface stains, it’s crucial to look past the myth that all discoloration signals neglect. Understanding the diverse origins of tooth stains—from our dietary habits and medications to the very process of aging and our genetic makeup—allows for a more informed and less judgmental perspective on dental aesthetics. Instead of self-blame, seeking professional dental advice empowers individuals to find the right solutions for their unique smiles.